
Gearing up for 2014: The looming health care reform provisions and your employee communication
 Now that the Supreme Court ruling and the November election are behind us, or mostly behind us, the big provisions of health care reform can no longer be put off. No doubt about it, January 1, 2014, is a big day for all employers but just one more step down a very long road that started in April 2010.
Now that the Supreme Court ruling and the November election are behind us, or mostly behind us, the big provisions of health care reform can no longer be put off. No doubt about it, January 1, 2014, is a big day for all employers but just one more step down a very long road that started in April 2010.
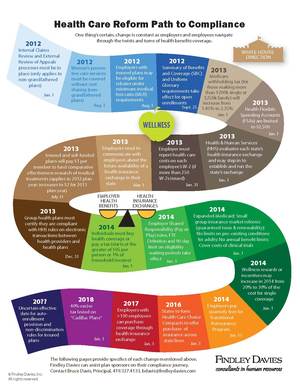
While the details are still overwhelming, this graphic does a great job showing the long, complicated road we’ve already been down and what’s ahead. What’s next? Assuming you’ve already taken care of your 2012 W-2s due out in January 2013, the next deadline is a legal disclosure just 57 working days away.
The view at 5,000 feet
Before we can get to that disclosure, let’s look at January 1, 2014. (We’ll try to do this succinctly!) In essence, it’s the date when all Americans need to have health insurance or pay a penalty (individual mandate). Since not all Americans have access to group plans, like employer-sponsored coverage or government programs, a few other provisions take effect.
- No matter your current health, you can’t be denied coverage (no more limits on pre-existing conditions).
- Businesses with at least 50 eligible employees must start offering affordable insurance starting in January 2014 or pay a penalty (pay or play).
- Health insurance exchanges must be set up in each state, where people can compare plan options based on price, benefits and services, and quality. And this is going to be messy! States have a choice on how to set up the exchanges. A state can establish it themselves, or appoint an agency. Or it may partner with the federal government. Some states are choosing to opt out of the exchanges altogether, which means the federal government will need to step in and run it for them.
March 1, 2013: Current deadline to send legal notice about the availability of the state exchanges
ACA mandates that employers send a legal notice about the availability of state exchanges. The DOL hasn’t released proposed regulations yet. The good news: based on the typical cycle (proposed regulations followed by a public comment period followed by the final regulations), we should get a few months to act once the DOL gets the process started. And we, for one, will be recommending that the DOL push out the deadline until late in the year so that most employers can send this notice to employees when they can actually take action—at enrollment time.
The not-so-good news: the information required in the notice is going to take a lot more work—and is going to be complicated for employers of all sizes. So, no matter what deadline the DOL ultimately sets, you’re going to want to get this into your plan for 2013.
You need to announce three things
(See section 1512 of the final law for the exact language.)
- State exchange basics: A description of the state exchange, what services the exchange provides and how to contact the exchange—meaning the website and customer service number. As you may know, not all states have decided how they’re going to comply. The Kaiser Family Foundation is keeping an updated map on where things stand. This is going to be challenging for multi-state employers.
- Your plan value: You need to tell employees if they will receive at least 60% coverage of essential health benefits—more on those in a minute—and if an employee might be eligible for a premium tax credit if they purchase a plan on the state exchange—more on this too.
- Tax implications: If an employee does purchase a health plan through the exchange, the money an employer contributes toward insurance will go away. Because the money an individual spent on employer-sponsored coverage is not taxed, buying coverage through the state exchange may change the individual’s tax obligation. And, as you know, employers will then not be able to deduct this coverage as a business expense.
Your homework
At a minimum, you need to know:
- Do you plans cover 60% of essential health benefits? The DOL issued proposed regulations just before the Thanksgiving break. Now you and your actuarial friends can discern if, in fact, you meet the minimum. If you don’t, you need to decide if or how to adjust your plan design to meet these minimums.
- Would any of your employees qualify for a premium subsidy? The government will provide a subsidy to households who have income equal to 100% to 400% of the federal poverty level AND don’t have access to the minimum coverage. Minimum coverage is a two-fold definition. It must cover 60% of essential health benefits, and single coverage must cost more than 9.5% of their family income. As you’re probably well aware, if an employee qualifies for a subsidy and gets it by purchasing coverage through the state exchange, you pay a penalty. Kaiser diagrams the penalty scenario clearly.
- The particulars on state exchanges. This one is out of your hands. But we are hopeful there will be a simple, streamlined way to communicate this (health.gov, for example) versus a requirement to provide details based on the state an employee lives in. This will be critical for companies with employees across the country.
Communicate your 2014 position before the legalese does
Clearly, once you figure out your strategy on plan design and how to comply with the 2014 provisions, you’ll need a strategic communication plan to bring employees along. You’ll need to get ahead of the legal notice with language that fits the notice into your big picture approach to health care reform compliance. For many employers, this strategy is going to include high-deductible health plans and incentive-heavy wellness programs, two benefit strategies that require robust, thoughtful communications in their own right.
Still more questions than answers
There are lots of guesses about how the employer-sponsored marketplace might change as a result of all the 2014 provisions. While we see employer-provided health insurance continuing, there will certainly be big changes—and some winners and some losers. Wellness will continue to be a dynamic arm of health benefits, as incentives increase.
There is also a lot left to untangle—from state exchanges to plan design to the actual content of required legal notices. As we’ve always done with health care reform, we’ll be here with you and help you make this as much a strategic opportunity as possible.
More resources
- Read the final regulations and guidance on the exchanges.
- Read the proposed regulations for wellness program incentives.
- Find out the top things small businesses need to know about the exchanges.
- NPR explains the basics of health exchanges.
- What are your responsibilities as an employer? Get a high-level overview.
- How will your state handle the exchanges? Get a state-by-state look at what your legislators are doing.
- Helping your state establish its SHOP? This guide provides government and business leaders with a roadmap to setting up SHOPS.
Work with Us
We partner with organizations that value their people first. Let’s talk.

Jennifer Benz, SVP Communications Leader, has been on the leading edge of employee benefits for more than 20 years and is an influential voice in the employee benefits industry.
